My Thyroid Lab Results Are Within Normal Range but I Still Don’t Feel Right?
At the Center for Occupational and Environmental Medicine (COEM), Board Certified Dr. William J. Weirs, MD, and Dr. Stephen P. Elliott, MD, specialize in uncovering the root causes of persistent thyroid symptoms. Even when standard lab results appear within the normal range, our physicians look beyond basic testing to identify underlying hormonal imbalances and environmental triggers. By combining clinical expertise with a personalized functional medicine approach, we provide comprehensive care tailored to your unique biochemistry. Trust Dr. Weirs and Dr. Elliott to help you reclaim your energy and achieve optimal health through advanced diagnostic insights. For more information, contact us today or schedule an appointment online. We are conveniently located at 7510 North Forest Drive North Charleston, SC 29420. Patients routinely fly in to be evaluated by COEM, as we serve patients internationally. Find out if you have been exposed, extensive lab testing is available.
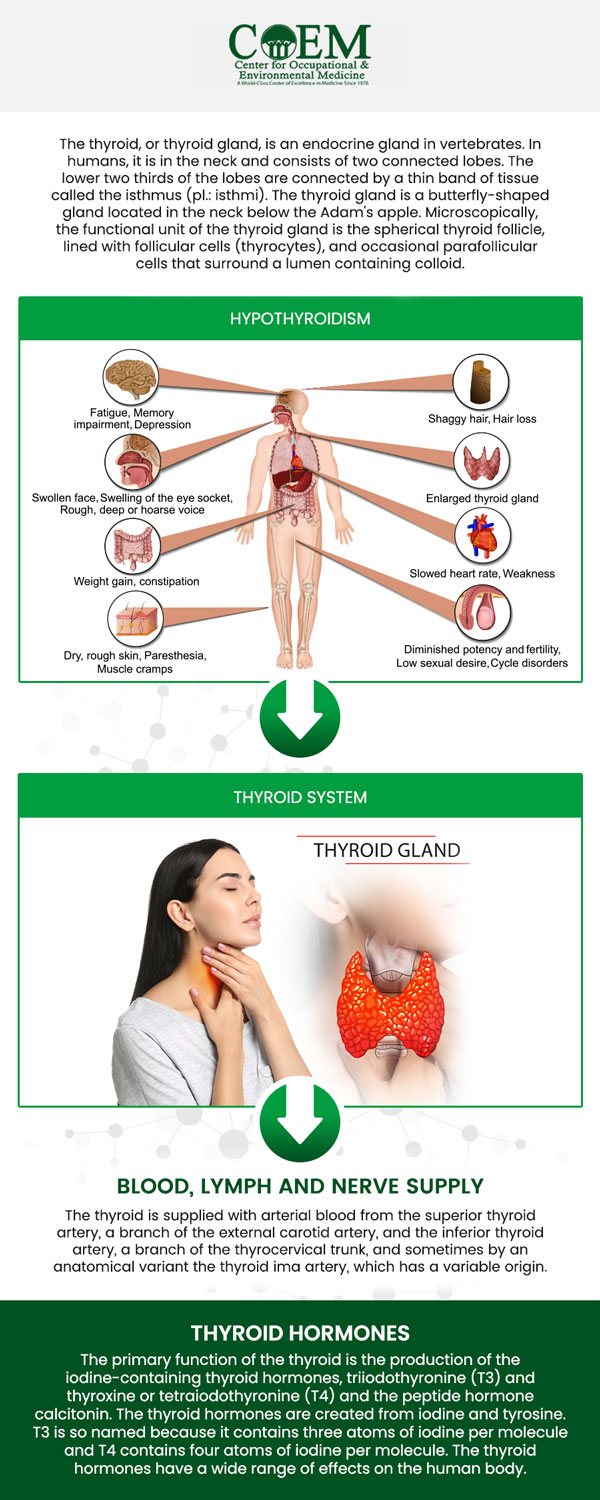
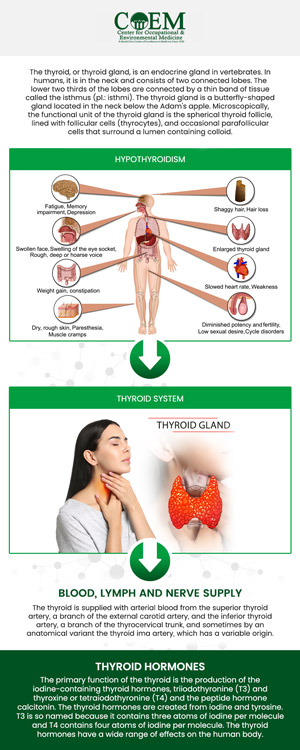
Table of Contents:
Can I still have thyroid issues if my lab results are normal?
Should I ask my doctor to test more than just TSH if my symptoms persist?
What are some common symptoms of thyroid problems, even with normal lab results?
What other conditions could be causing symptoms that mimic thyroid problems?
Thyroid Health and Ongoing Symptoms: How Dr. William J. Weirs, M.D. & Dr. Stephen P. Elliott, M.D. Can Help
A patient can continue to experience thyroid issues or similarly presenting symptoms even when standard laboratory markers appear normal. In many primary care settings, thyroid screening is limited to TSH. TSH offers a regulatory signal from the brain to the thyroid, but it does not always reflect the full scope of thyroid hormones. An individual may present with fatigue, weight fluctuation, hair thinning, mood instability, or cold sensitivity while being told that the results are normal. Thyroid physiology is layered and requires thorough evaluation. Free T4 reflects circulating storage hormone, free T3 represents the active form at the cellular level, and reverse T3 can indicate altered conversion patterns during stress or illness. Antibodies may reveal autoimmune activity even before overt dysfunction appears in routine testing. A person can remain within statistical norms while still experiencing issues.
The specialists at The Center for Occupational and Environmental Medicine (COEM) take into account this complexity when evaluating ongoing symptoms. Their approach considers thyroid balance within the overall hormonal and metabolic network. A patient with persistent complaints may require deeper assessment to uncover patterns that standard screening overlooks. Functional medicine evaluation looks at how thyroid signaling interacts with adrenal regulation, nutrient status, inflammation, and environmental influences.
When symptoms continue despite a normal TSH, expanding the evaluation may provide clarity. TSH measures the signaling loop between the pituitary gland and the thyroid, yet it does not directly measure everything. A more comprehensive panel at COEM can include free T3, free T4, reverse T3, and thyroid antibodies. Each marker offers a different layer of information about production, conversion, immune involvement, and overall thyroid performance.
Persistent symptoms are often indicative of larger system stress. Nutrient deficiencies such as iodine, selenium, iron, and zinc can influence hormone synthesis and conversion. Chronic inflammation, gut imbalance, and environmental exposures may interfere with receptor sensitivity or increase autoimmune activation. Evaluating additional markers can help reveal whether the issue lies in hormone production, peripheral conversion, immune response, or systemic stress load.
At COEM, providers integrate comprehensive thyroid panels into a thorough metabolic assessment. This process involves reviewing hormonal balance, inflammatory markers, nutritional status, and environmental factors that may burden the endocrine system. By examining a full range of thyroid markers alongside lifestyle and environmental influences, clinicians can develop a more individualized plan.
Individuals who report thyroid symptoms often describe persistent fatigue that does not resolve with rest. Cognitive slowing, difficulty concentrating, and mood shifts may also appear. Some patients experience dry skin, brittle nails, hair thinning, constipation, or unexplained changes in weight. Sensitivity to cold, menstrual irregularities, and reduced exercise tolerance are also frequently reported. These symptoms can arise when hormone signaling at the cellular level is inefficient, even if circulating levels appear normal. Conversion from T4 to T3 may be altered during periods of chronic stress or inflammation. Elevated reverse T3 may reflect a metabolic adaptation to stress. Autoimmune activity can be present before overt hormone decline, creating subtle but impactful changes in energy and regulation.
Metabolic balance depends on more than hormone production alone. Blood sugar instability, sleep disruption, and adrenal strain can amplify thyroid-related complaints. Poor digestion may reduce nutrient absorption, limiting the building blocks required for proper hormone synthesis. Environmental exposures such as heavy metals or endocrine-disrupting chemicals may further complicate regulation. Specialists at COEM work to determine whether thyroid signaling inefficiencies are contributing to the patient’s overall health concerns.
A range of conditions can mimic thyroid dysfunction. Chronic fatigue related to adrenal dysregulation may produce low energy, brain fog, and mood variability. Blood sugar imbalance can contribute to shakiness, irritability, and fluctuating energy levels. Nutrient deficiencies such as low iron or vitamin B12 may cause hair thinning, weakness, and cognitive changes that overlap with thyroid complaints.
Autoimmune activity elsewhere in the body may also create systemic symptoms. Chronic infections, gut dysbiosis, and inflammatory disorders can alter metabolism and mimic an endocrine imbalance. Hormonal fluctuations involving estrogen or cortisol may present with weight changes, sleep disruption, and temperature sensitivity. Environmental toxin exposure may further complicate metabolic signaling.
At COEM, complex chronic illness is approached with detailed diagnostic panels and outcome tracking. This evidence-based strategy allows clinicians to differentiate thyroid dysfunction from other overlapping conditions.
Dr. William J. Weirs board certified in emergency medicine, and Dr. Stephen P. Elliott, the only MEDMAPS-certified physician in the region, bring an evidence-based framework to patients with complex chronic presentations. Their evaluations extend beyond standard screening and incorporate comprehensive thyroid panels, metabolic markers, inflammatory indicators, and immune assessment. This layered approach supports a more accurate understanding of endocrine performance.
Functional medicine principles guide their assessment process. They review the patient’s health history, environmental exposures, dietary patterns, stress load, sleep quality, and toxin burden. By identifying contributors such as nutritional deficiencies, chronic inflammation, infections, or hormonal imbalance, they aim to reduce the systemic pressures that strain thyroid regulation. Addressing gut health and adrenal balance frequently plays a central role in restoring endocrine stability.
Ongoing monitoring allows for careful adjustment of targeted therapies. Laboratory trends are correlated with symptom progression, ensuring that interventions are aligned with measurable outcomes. Lifestyle modifications, including nutrition planning, stress management strategies, and environmental exposure reduction, are integrated into each plan. This proactive model seeks to stabilize thyroid function before more advanced dysfunction develops.
Through comprehensive assessment and personalized care at COEM, patients with unresolved thyroid-related concerns receive a broad evaluation of interconnected systems to identify the root cause of their issues. For more information, contact us today or schedule an appointment online. We are conveniently located at 7510 North Forest Drive North Charleston, SC 29420. We serve patients from Charleston SC, Mount Pleasant SC, Summerville SC, North Charleston SC, Goose Creek SC, Ladson SC, Hanahan SC, James Island SC, John’s Island SC, Daniel Island SC, West Ashley SC, Moncks Corner SC, Sullivans Island SC, Folly Beach SC, Isle of Palms SC and all of South Carolina, Nationally, and Internationally. Patients routinely fly into Charleston to be evaluated by COEM and to enjoy this beautiful city, which is a Condé Nast and Travel and Leisure Top Domestic and International Tourist Destination.

Check Out Our 5 Star Reviews


Additional Services You May Like
- Functional Medicine
- Allergy and Autoimmunity
- Asthma and COPD
- Autoimmune Diseases
- Allergy and Immunology
- Anti Aging Medicine
- Autism and Children
- ADHD
- Bacterial Infections
- Chemical Toxicity
- Candida Fungal Problems
- Cancer Treatment
- Chronic Illness
- Chronic Inflammatory Response Syndrome (CIRS)
- Chronic Fatigue
- Cardiovascular Disease
- Carbon Monoxide Poisoning
- Chelation Therapy
- Depression
- Environmental Medicine
- Ear Ringing and Dizziness
- Fatigue Treatment
- Fertility and Preconception Care
- Gut Health
- GI 360 Test
- Heavy Metal Toxicity
- Hormonal Imbalances
- Headaches and Migraines
- Hormone Balancing (Men & Women)
- Hepatitis
- Integrative Medicine
- Independent Medical Evaluations
- Influenza
- Lab Testing
- Mold Toxicity
- Malnutrition
- Neurodegenerative Disease
- Natural Hormone Balancing For Women
- Preservative-Free IV Therapy
- Stomach Acid Imbalance
- Smoking Cessation Program
- Skin Therapy (Anti-Aging)
- Swine Flu
- Thyroid
- Mold Toxicity
- Vitamin D
- Weight Loss Program
- Women’s Breast Health Formula

Additional Services You May Like
- Functional Medicine
- Allergy and Autoimmunity
- Asthma and COPD
- Autoimmune Diseases
- Allergy and Immunology
- Anti Aging Medicine
- Autism and Children
- ADHD
- Bacterial Infections
- Chemical Toxicity
- Candida Fungal Problems
- Cancer Treatment
- Chronic Illness
- Chronic Fatigue
- Cardiovascular Disease
- Chronic Inflammatory Response Syndrome (CIRS)
- Carbon Monoxide Poisoning
- Chelation Therapy
- Depression
- Environmental Medicine
- Ear Ringing and Dizziness
- Fatigue Treatment
- Fertility and Preconception Care
- Gut Health
- GI 360 Test
- Heavy Metal Toxicity
- Hormonal Imbalances
- Headaches and Migraines
- Hormone Balancing (Men & Women)
- Hepatitis
- Integrative Medicine
- Independent Medical Evaluations
- Influenza
- Lab Testing
- Mold Toxicity
- Malnutrition
- Neurodegenerative Disease
- Natural Hormone Balancing For Women
- Preservative-Free IV Therapy
- Stomach Acid Imbalance
- Smoking Cessation Program
- Skin Therapy (Anti-Aging)
- Swine Flu
- Thyroid
- Mold Toxicity
- Vitamin D
- Weight Loss Program
- Women’s Breast Health Formula